DuxWare Release Note - 09/04/2015 - (ICD-10 Readiness & Testing Guide, Appointment Schedule updates
Contents
Release Note - 09/29/2015
ICD-10 Readiness:
Have you completed a checklist list of tasks to complete before ICD-10 implementation 10/1/2015?
Keep in mind there are quite a number of items to have completed before ICD-10 implementation. So, there's a little more to the process than changing your ICD codes from 9 to 10 to file your claims. An excellent resource is the CMS.gov/ICD10 web site: https://www.cms.gov/Medicare/Coding/ICD10/index.html
What will happen in your Practice Management System on 10/1/2015?
All payers will be set to accept ICD-10 level codes only. Check with your clearinghouse for payers that are NOT ready for ICD-10. If you have a payer that is not ICD-10 ready, you will need to manually go into the Payer Setup and select ICD Level: ICD-9.
What if I need to file claims with service date(s) prior to 10/1/2015, and my payer is set to ICD-10?
If your payer has been set to only accept ICD-10 codes, you can still file or refile claims with ICD-9 codes with service dates prior to 10/1/2015 thus eliminating the need to switch the payer ICD Levels back and forth between ICD-10 and ICD-9.
An ICD-9 to ICD-10 Cross-walk is available to you at Claim Entry and in the Diagnosis Management Section of your PM
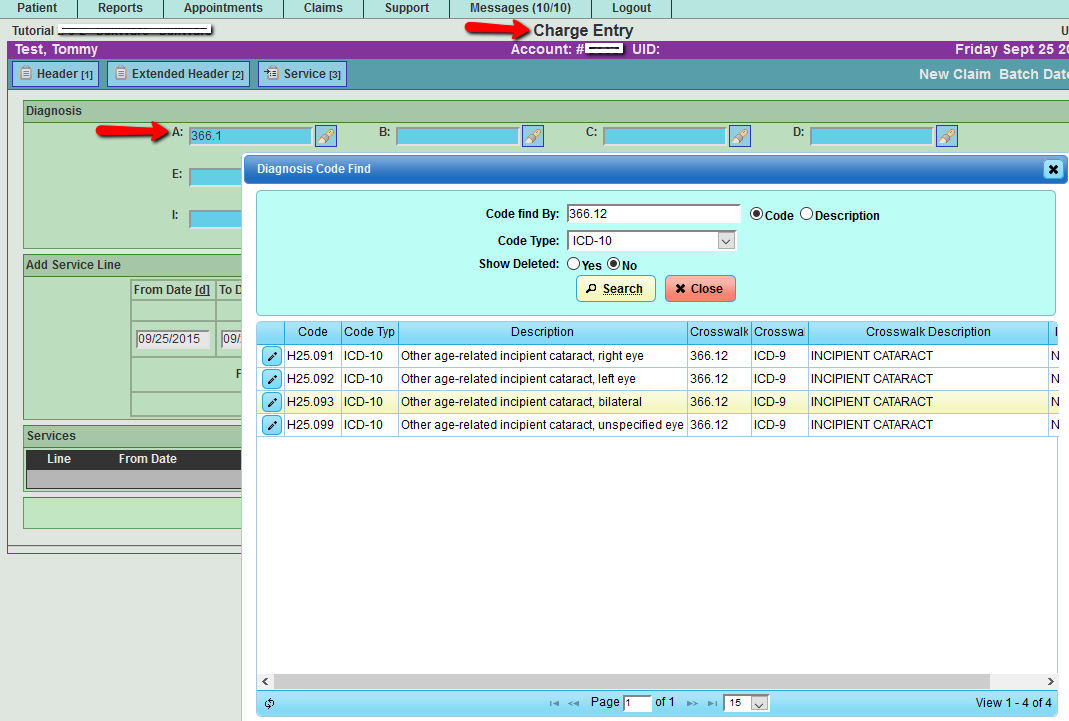
If you are manually entering a claim with an ICD-9 code, and the payer level is set to ICD-10, you will be presented with an ICD-9 to ICD-10 cross-walk to help you select from a list of corresponding ICD-10 matches to the ICD-9 code. Keep in mind that your choice of ICD-10 code should reflect the diagnosis at encounter.
ICD-9 to ICD-10 Crosswalk takes the ICD-9 code and presents a pop-up with the possible ICD-10 matches as illustrated below. You simply select the ICD-10 code and move to the next ICD field.
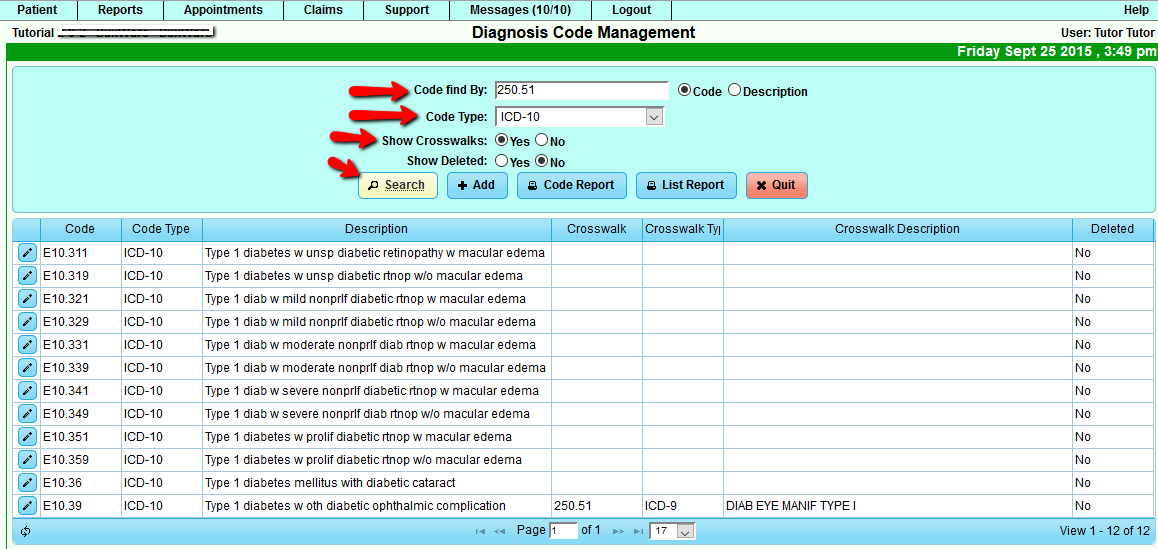
To access Diagnosis Code Management from the Support tab: Support>Diagnosis/Procedure>Diagnoses:
ICD-10 to ICD-9 Cross-walk
All of your claims are coded with ICD-10 codes automatically via interface from your EMR. Your Practice Management system is set to detect payers that do not accept ICD-9 codes based on your selection in the Payer Setup. ICD-10 codes will automatically cross-walk down to the ICD-9 code match.
Important System Update for 10/2/2015
Please select the link below for Charge Entry Updates
ICD-9 Override
ICD-10 Practice Management Testing Guide
Click the link below to access your ICD-10 Practice Management Testing guide:
Testing your Electronic (837) claims for ICD-10 Readiness
Appointment Schedule Update
Extended Slots/Consuming Slots:
Consuming slots is a new feature that allows the practice to determine how many appointment slots to consume by Appointment Type and/or Appointment Category. If you are consuming slots in both Appointment Type and Appointment Category, the type or category with the most number of slots consumed will override the the appointment type or category with the lesser slot consumption.
Click the link below to access the guide:
[Type, Appointment Category, & Recall Category Setup]
Payer Setup Option - Texas Worker's Compensation
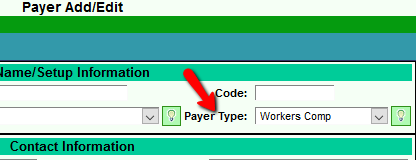
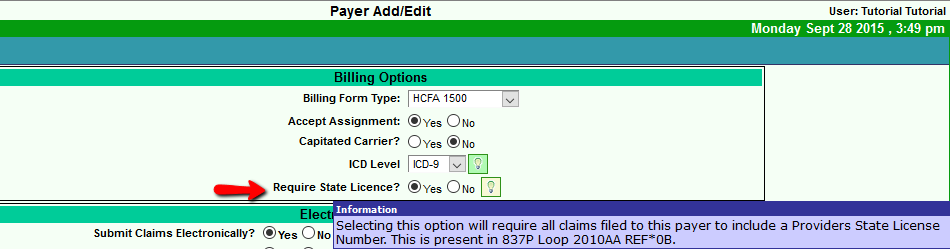
There is a new option in the Payer Setup to accommodate Texas Worker's Compensation Requirements to include a Referring Provider's state license number on electronic and paper claims. This option eliminates teh setup of the Referring Provider Payer Link. The payer should set to Payer Type: Workers Compensation. On the "Billing Page", select "yes" to pull in the Provider's state license, and "Save" your change. This will retrieve the Referring Provider's state license number if entered in the Referring Provider's record.
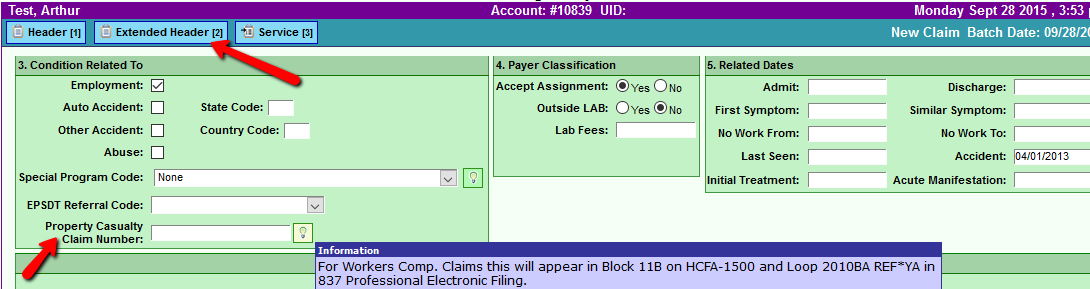
At Claim Entry, enter the Worker's Compensation Claim Number assigned by the payer:
Please feel free to contact us via e-mail at support@duxware.com or by telephone at 1-800-248-4298 if you have any questions.