DuxWare Release Note - 10/2/2015
Release 10/2/2015
Attention - ICD-9 charge entry: Your system has been modified to automate the ICD-10 to ICD-9 down conversion process that is necessary to bill claims prior to 10/01/2015 as well as claims that are filed to payers not accepting ICD-10 coding. This automation will use the GEM (General Equivalent Mappings) to down code ICD-10 to ICD-9 for such claims. The automation uses the ICD-9 code listed in your “crosswalk” for the ICD-10 code selected and will submit it in place of the ICD-10 code used on the claim. One use of this automation is to allow you to code the claim in ICD-10 to submit the claim primary to the payer that accepts ICD-10 codes. The same automation then submits the claim, with ICD-9 codes this time, to the secondary payer if the secondary payer does not accept ICD-10 codes on claims. This is done without you having to change the codes on the claim in order to file it correctly.
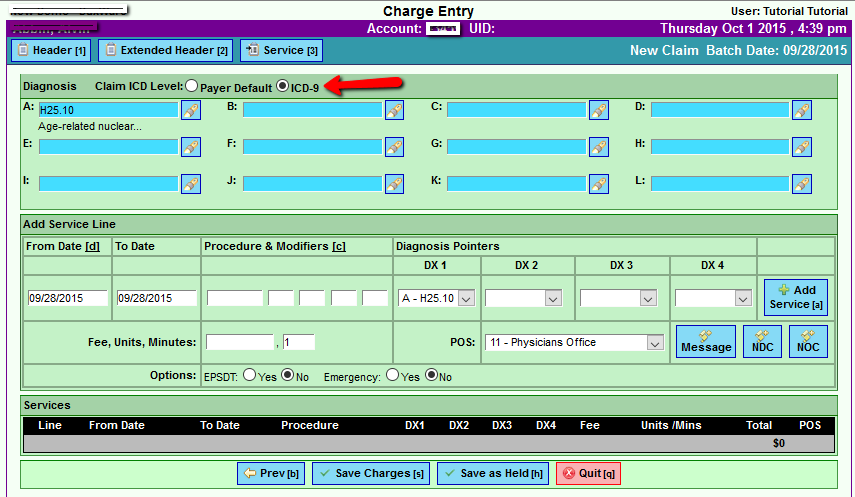
A new feature was added today that will speed up charge entry on claims with service dates prior to 10/01/2015 and any claims which require ICD-9 instead of ICD-10 codes. This procedure will bypass the automation mentioned above during the charge entry process. From the CHARGE ENTRY SCREEN, check the button in the Diagnosis section that says Claim ICD Level and change it to ICD-9. Note: the default for this feature is “Payer Default” which will utilize the ICD Level setting in the Payer Add/Edit screen for the payer on the claim you are creating. Next, continue populating the Diagnosis fields A – L as you normally would. If you know the proper ICD-9 code, simply enter it into the field and continue creating the claim as normal. If you want to search for the ICD-9 code, click the Flashlight Search button as normal and you will be able to search the ICD-9 codes in the system. Continue entering the claim details and process the claim as usual.
ICD-10 Workflow Effective 10/1/2015
Workflow #1 – Practice uses ICD-10 for ALL CLAIMS
- A. Claims filed to an ICD-9 level payer will use ICD-9 codes on
- a. HCFA 1500 02/12 (not 08/05 version) Form
- b. UB-04 Form
- c. 837P (Electronic Professional Claim)
- d. 837I (Electronic Institutional Claim)
- B. Claims Filed to an ICD-10 level payer will use ICD-10 codes on
- a. HCFA 1500 02/12 (not 08/05 version) Form
- b. UB-04 Form
- c. 837P (Electronic Professional Claim)
- d. 837I (Electronic Institutional Claim)
Workflow #2 – Practice uses ICD-9 for claims PRIOR to 10/1/2015
- A. Claims filed to ICD-9 level Payer will use ICD-9 codes
- B. Claims filed to ICD-10 level Payer will use ICD-9 codes
Workflow #3 – Practice uses ICD-9 for claims ON or AFTER 10/1/2015
- A. An Error appears:
- a. Oct. 1st, 2015, ICD-10 codes must be used
- i. In Claim Manager – goes to error tab with above message.
- ii. For HCFA Print – PDF with error is created
- iii. For UB-04 Print – PDF with error is created
- a. Oct. 1st, 2015, ICD-10 codes must be used
Workflow #4 – Practices that do not bill to Governmental or Commercial Payers On or AFTER 10/1/2015
- A. Practice has the option to request that the PM switch all payers back to ICD-9 level.
- a. Practice will still have the option to select ICD-10 level in payer setups on a case by case basis.